Waking up to a nighttime killer
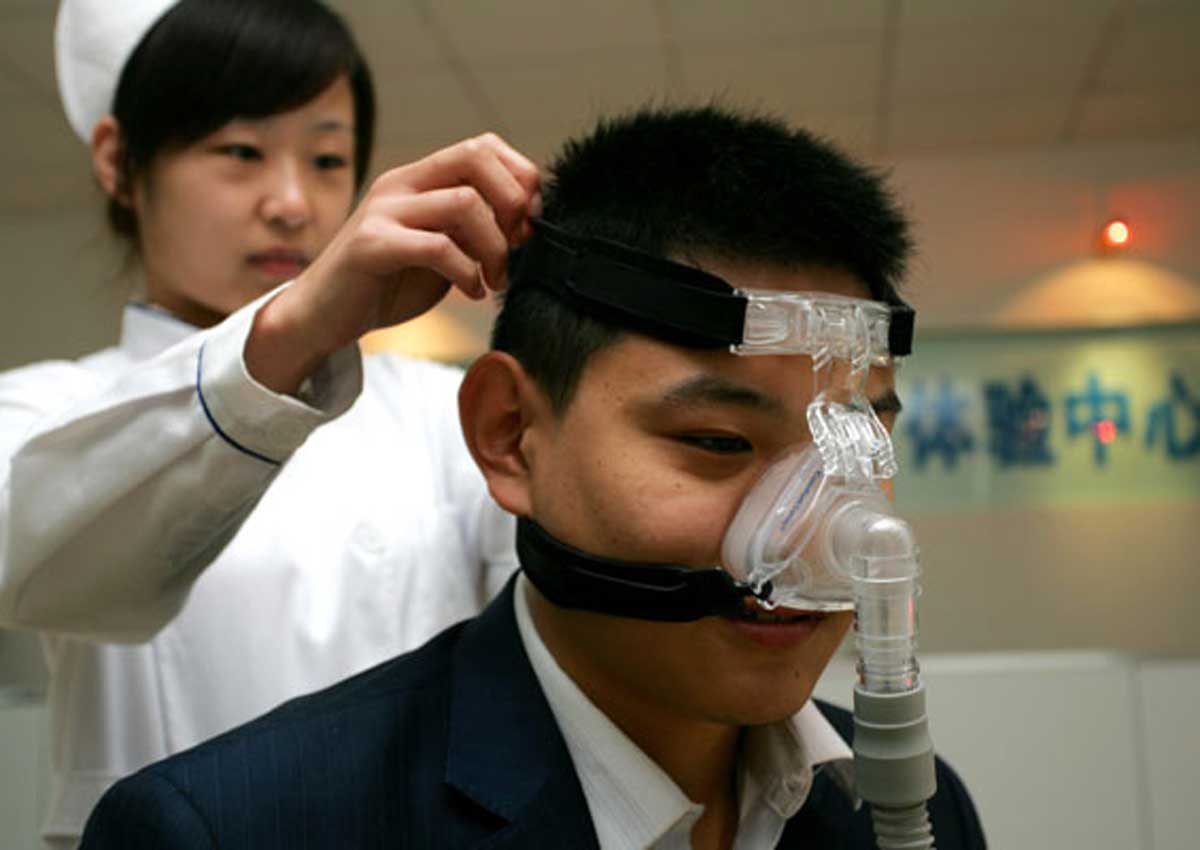
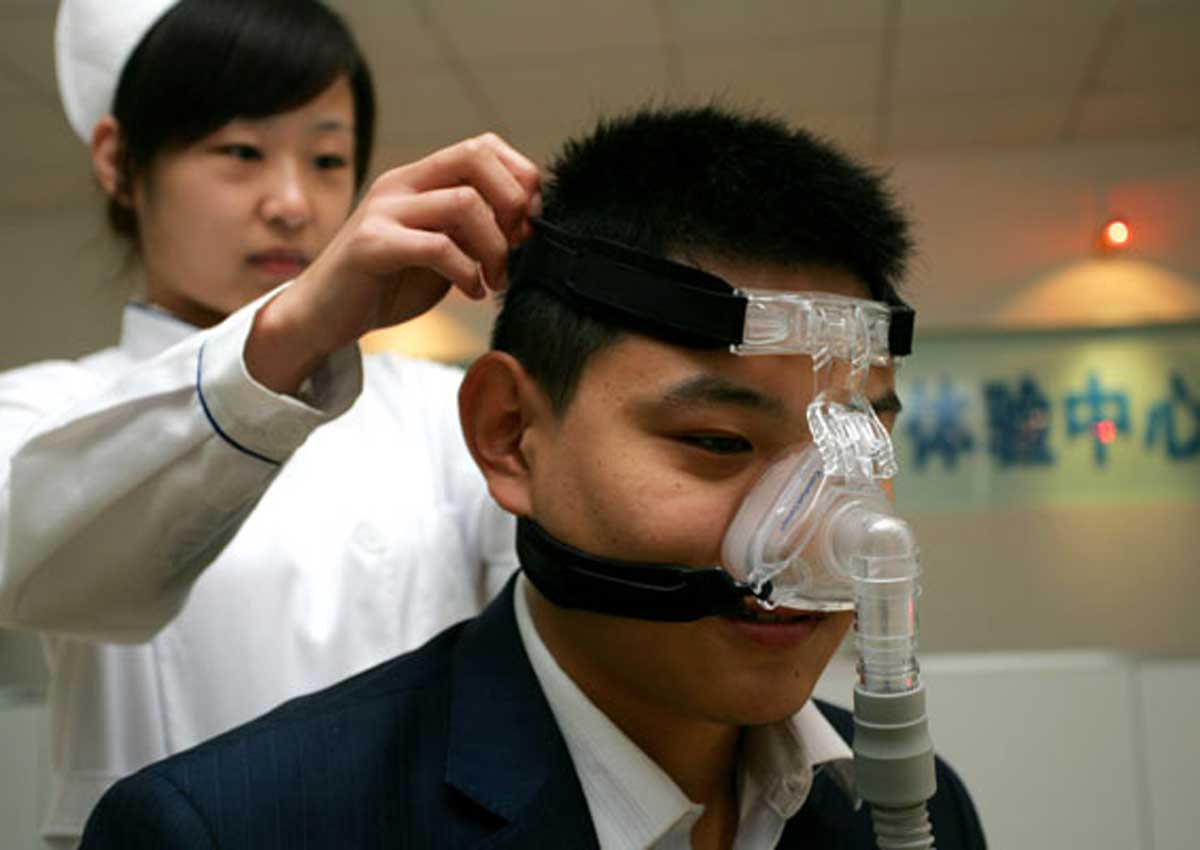
Home testing kits for sleep apnea are cutting hospital waiting times and helping patients recover faster.
Kong Siu-ki used to regularly wake up on mornings feeling as exhausted as when he went to bed the night before. He rarely slept well. Neither did his family, as his loud snoring could rattle the dishes.
Yet this portly, 54-year-old man simply dismissed it as one of life’s little irritants. He would go through the day tired and listless, never grasping that his sleep difficulties were destroying his health.
A lack of sleep affects the body’s normal healing processes and cognitive functions, leaving a person accident-prone or hyperactive. Research has also found sleep-deprived individuals process glucose more slowly, which increases the risk of Type 2 diabetes, and have a shorter-than-average life span.
Kong was obese, diabetic and had high blood pressure. Yet it was only in November, when he consulted doctors about getting laparoscopic surgery-an adjustable gastric band around the stomach-to lose weight, that he learned the terrifying ramifications of his loud snoring.
Doctors suspected he had obstructive sleep apnea, a disorder in which people have paused or shallow breathing during sleep. One doctor issued a stark warning: Kong would need anaesthesia to go under the knife, but if the sleep apnea was left untreated, the anesthetic could soften his throat muscles, blocking his airway, which could kill him.
“I had no idea. I was overweight, drowsy and snored louder than other people, but I thought that was all,” Kong said.
David Hui Shu-cheong, head of medicine and therapeutics at the Chinese University of Hong Kong, who specializes in respiratory medicine, stressed that one of the biggest risk factors associated with sleep apnea is obesity.
Anyone with a large neck is at risk. Then there are other issues like smoking and alcohol that only make things worse, he said.
THE HOPE AT HOME
Kong was referred to a respiratory specialist at Prince of Wales Hospital and advised to undergo a diagnostic sleep test, known as a polysomnography.
However, the average waiting time for the test at a public hospital in Hong Kong is 72 weeks. Doctors did not feel it was safe for Kong to wait that long, so in December, they recommended he perform a sleep test at home using a monitor called an Embletta.
When he did, the results were unsettling. The device recorded that he stopped breathing 58 times every hour, each time for at least 10 seconds. He was diagnosed with severe sleep apnea.
Prince of Wales Hospital is the only public hospital in the city that offers to lend machines to patients suspected of having sleep disorders, saving them the hassle of an overnight stay at its clinic. Hui, who introduced the idea, believes it could be a long-term solution to easing the pressure on an overburdened public healthcare system.
In Hong Kong, five in every 100 middle-aged men have sleep apnea. More men have it than women, Hui said. “More middle-age men are now obese. The increased neck fat can clog the airways, resulting in snoring and pauses in breathing, which meets the definition for sleep apnea.”
Every year, Prince of Wales Hospital treats more than 1,000 patients who display signs of sleep apnea. About 400 take the diagnostic tests at home, after doctors have given them instructions on the machine, with the rest admitted to hospital.
“Despite many patients awaiting the test, we have only four beds for them,” Hui said. “If we hadn’t initiated the programme, the waiting time would be much longer.”
The home-based approach in treating milder chronic diseases has shown benefits for patients and front-line medical workers. One example is the continuous positive airway pressure therapy, or CPAP, given to sleep apnea patients.
Kong was one of hundreds selected to receive home-based therapy last year. In January, he was given a CPAP machine with a tight-fitting face mask to conduct overnight CPAP titration, the first step in alleviating sleep apnea. It allows doctors to assess the optimal air pressure needed to keep a patient’s airway open during future CPAP treatments.
The conventional diagnosis for sleep apnea entails a two-night stay at a hospital: First for the sleep test, then for the CPAP titration. The average cost of the procedure for those who take the test at home is HK$8,479 ($1,080), about 60 per cent less than for those who are admitted to hospital.
After the initial diagnosis, both sets of patients need to buy a CPAP machine to conduct the long-term therapy at home.
Not only does the home-based approach save time and money, it has been proven to yield better therapeutic results, according to a study by the Chinese University of Hong Kong, which compared the differences in patients receiving ambulatory care and hospital care.
The study, carried out between September 2013 and August 2014, involved 172 patients with moderate to severe sleep apnea. It found those who received the test and CPAP titration at home were more responsive to treatment.
“Sleep apnea patients felt more restful when sleeping in their own beds rather than at hospital,” Hui said. “In familiar settings, subjects became acclimated to the CPAP machine at home quicker.”
The study also showed the average waiting time between the first consultation and the diagnostic sleep test was cut by more than 75 per cent for patients receiving ambulatory care. Plus, these patients also reported a decrease in daytime lethargy and better cognitive functions.
Kong uses his CPAP machine every day now. He said he is sleeping better, and on nights he stops breathing only about four times an hour, a marked improvement.
“I can finally go into deep sleep,” he said. “I feel rested during the day, and what’s more, my blood pressure has retreated to a normal level.”
Published at Sat, 09 Sep 2017 13:00:00 +0000